
Dr. Swapan Kumar De
Senior Most Interventional Cardiologist at
Apollo Multispeciality Hospital Kolkata.
MD, DM (Cardiology)
EP Study Specialist in Kolkata, India



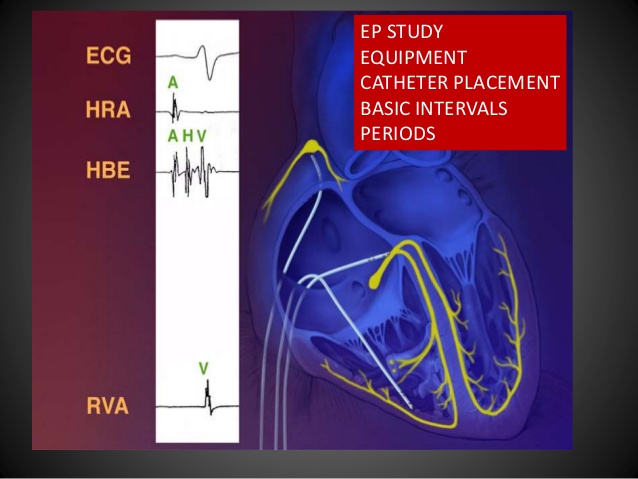
The electrophysiology study (EP study) is a special catheterization test, in which electrode catheters (flexible, insulated wires with metal electrode tips) are inserted in to the heart in order to study the cardiac electrical system. The cardiac electrical system is important, because it controls the heart rhythm and because abnormalities in the electrical system are responsible for most heart arrhythmias. Read more about the heart's electrical system here.
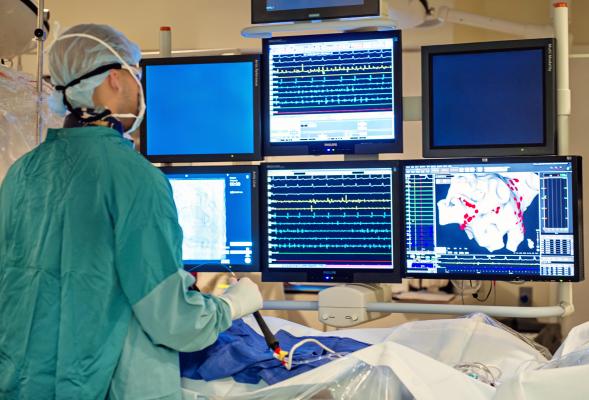
If you have an EP study, you will be brought to the electrophysiology laboratory (a specialized catheterization laboratory) and you will lie down on an examination table. You will be given local anesthesia, and possibly a mild sedative, and then electrode catheters will be inserted in to one or more blood vessels. (Catheters are inserted either through a small incision or by means of a needle-stick, usually in the arm, groin or neck. Most often two or three catheters are used, and they may be inserted from more than one site.) Using flouroscopy (similar to an x-ray), the catheters are advanced through the blood vessels and in to specific areas within the heart.
Once they are appropriately positioned, the electrode catheters are used to do two main tasks: to record the electrical signals generated by the heart and to pace the heart. (Pacing is accomplished by sending tiny electrical signals through the electrode catheter.) By recording and pacing from strategic locations within the heart, most kinds of cardiac arrhythmias can be fully studied.
Once the procedure is completed, the catheter(s) are removed. Bleeding is controlled by placing pressure on the catheterization site for 30 to 60 minutes.
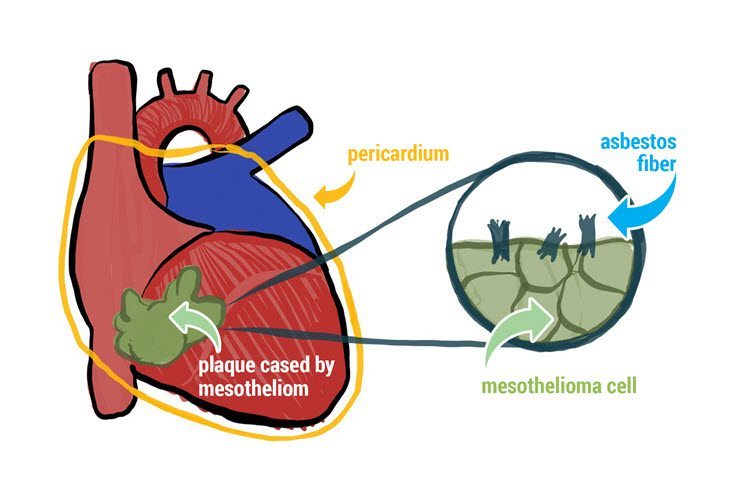
The EP study can help to evaluate both the bradycardias (slow heart arrhythmias) and thetachycardias (rapid heart arrhythmias).
If the EP study reveals a significant propensity for bradycardia, a permanent pacemaker may be required.
Tachycardias are assessed by using programmed pacing techniques to induce (i.e., to start up) the tachycardia. If tachycardias can be induced during the EP study, then by studying the electrical signals recorded from the electrode catheters, the precise cause of the tachycardia can usually be identified. Once this is accomplished, the appropriate therapy for the tachycardia usually becomes clear.
Insertion of a pacemaker: If the EP study confirms the presence of significant bradycardia, a permanent pacemaker can often be inserted immediately, during the same procedure.
Ablation: If supraventricular tachycardia (SVT) - and some forms of ventricular tachycardia (VT) - are found, radiofrequency ablation is often the treatment of choice. The ablation procedure is usually carried out during the same procedure, immediately following the EP study.
Implantable defibrillators: If rapid forms of VT and/or ventricular fibrillation (VF) are identified during the EP study, most commonly an implantable defibrillator is the treatment of choice. This device can now often be inserted in the EP laboratory, immediately following the EP study. In earlier years, the EP study was used to identify the "best" anti-arrhythmic drug for patients with VT or VF, but today it is known that no anti-arrhythmic drug is as effective as the implantable defibrillator in preventing sudden death from these arrhythmias.
The potential risks of having an EP study are similar to those of having a cardiac catheterization. These procedures are relatively safe, but because they are invasive procedures involving the heart, several complications are possible. You should not have an EP study unless there is a reasonable likelihood that the information gained from the procedure will be of significant benefit.
Minor complications include minor bleeding at the site of catheter insertion, temporary heart rhythm disturbances caused by the catheter irritating the heart muscle and temporary changes in blood pressure.
More significant complications include perforation of the heart wall (causing a life-threatening condition called "cardiac tamponade"), extensive bleeding or (because potentially lethal arrhythmias are being induced) cardiac arrest. The risk of dying during an EP study is less than 1 out of 1,000.
An electrophysiology (EP) study is a test that records the electrical activity and the electrical pathways of your heart.
It can help find what's causing your irregular heartbeat. It also helps figure out the best treatment for you.
During the EP study, your doctor will safely reproduce your heart rhythm. Then, they may give you different medicines to see which controls it best.
Sometimes, one of these studies is done before you get an implantable cardioverter/defibrillator (ICD). It can help your doctor discover which device is best for you. It can also help them track treatment success.
EP study is a test which looks at your heart's electrical activity in more detail.
It's used to diagnose and treat a wide variety of abnormal heart rhythms.
An EP study can stimulate and diagnose abnormal heart rhythms and identify which areas of your heart are affected.
If the cause of your abnormal heart rhythm is found, the doctor will sometimes proceed to treat the problem by doing a catheter ablation. This treatment uses either heat (radio-frequency ablation) or freezing (cryogenic ablation) to destroy the areas inside the heart which are causing the abnormal rhythm and therefore relieve the symptoms. This may be done at the same time as the EP study.
EP) study is a test performed to assess one's heart's electrical system or activity and is used to diagnose abnormal heartbeats or arrhythmia.
The test is performed by inserting catheters and then wire electrodes, which measure electrical activity, through blood vessels that enter the heart.
When you arrive at the hospital, the final steps to prepare for the EP study are:
1. For your comfort, empty your bladder as completely as possible. A bedpan or urinal will be available during the procedure. Depending on the length of your precedure, a catheter may be inserted to drain your bladder of urine during the procedure.
2. A small intravenous (IV) needle will be inserted into a vein in your arm to administer drugs, if necessary.
About Cardiologists : Cardiologists treat people with diseases or conditions of the heart and people who want to learn the risk factors for heart disease. A primary care doctor or family practice doctor can work with a cardiology specialist to diagnose, treat, and manage heart conditions and help people make heart-healthy lifestyle choices. Patients who are at risk for heart disease or have a history of heart symptoms may see a clinical cardiologist regularly. People with ongoing heart conditions, pacemakers, or frequent heart trouble are likely to see a cardiologist with a subspecialty.